 The height of the waveform depends on the amount of CO2 detected, and the length of the waveform depends on the time of exhalation. A sharp downward spike is then seen during inhalation. A sharp spike is normally seen when exhaled air from the alveoli reaches the sensor, and plateau’s when all of the exhaled air detected came from the alveoli. There is normally no CO2 present in dead space, and the graph should be at baseline. The waveform starts at the beginning of exhalation, and senses air from dead space in the upper airway and bronchi. The capnography waveform represents air movement in the lungs, similar to how complexes on an ECG represent electrical conduction through the heart. Adding waveform capnography to history and physical exam findings can help with treatment decisions. A number of conditions can cause diminished breath sounds, wheezing may be heard with both asthma and pulmonary edema, and crackles may be heard with pulmonary edema and pneumonia. Capnography helps diagnose the cause of respiratory distressĬorrectly diagnosing the cause of respiratory distress can be difficult, and treating the wrong condition may cause harm. An elevated capnograph in this group of patients means that their effort is not effectively eliminating CO2 (hypercarbia) They may be progressing to respiratory failure from hypercarbia and fatigue, not hypoxia, and need assisted ventilation.ģ. It is important to understand that patients in respiratory distress may inhale enough oxygen and have a normal pulse-ox reading, but still struggle to get air out. Patients with asthma, COPD, CHF, and pneumonia must often exert themselves to exhale with accessory muscles. While a rise in CO2 should stimulate someone to breathe, no effort should be needed to exhale it. Conversely, if an unresponsive patient has a normal ETCO2, a conservative approach with close monitoring can be taken. Pulse oximetry helps determine how much oxygen should be administered, and capnography helps determine when ventilation should be assisted with a bag valve mask. This may be caused by an overdose, head injury, or seizure. If a patient has slow or shallow respirations, and a high ETCO2 reading, this tells us that ventilation is not effectively eliminating CO2 ( hypercarbia), and that the brain is not responding appropriately to CO2 changes. The patient’s respiratory rate should increase as CO2 rises, and decrease as CO2 falls. ETCO2 adds an objective measurement to those findings. We assess this by observing chest rise and fall, assessing respiratory effort, counting respiratory rate, and listening to breath sounds. In people with healthy lungs, the brain responds to changes in CO2 levels in the bloodstream to control ventilation. ETCO2 provides clues about respiratory effort Pulse-oximetry assess oxygenation, and works by measuring the how much of each red blood cell is bound with oxygen. Ventilation is the air movement in and out of the lungs, while oxygenation is the amount of oxygen inhaled by the lungs that reaches the bloodstream. In patients who require assisted ventilation, another adapter can be attached to a BVM and advanced airway device.Ĭapnography assesses ventilation, which is different from oxygenation. Those prongs can also be used to administer a small amount of oxygen, or applied underneath a non-rebreather or CPAP mask. In patients who are breathing, nasal prongs can be applied that capture exhaled air. Two sensors can be used to measure capnography. 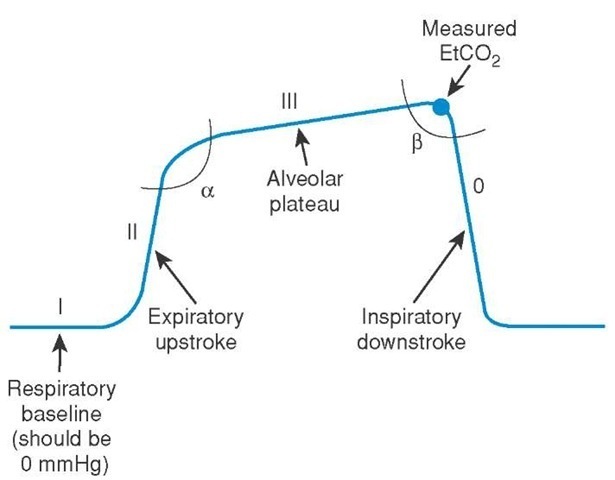
Changes in respiratory rate and tidal volume are displayed immediately as changes in the waveform and ETCO2. Capnography also measures and displays respiratory rate. The capnograph is the waveform that shows how much CO2 is present at each phase of the respiratory cycle, and it normally has a rectangular shape. This is end-tidal CO2 (ETCO2) which is normally 35-45 mm HG. The number is capnometry, which is the partial pressure of CO2 detected at the end of exhalation. Waveform capnography represents the amount of carbon dioxide (CO2) in exhaled air, which assesses ventilation. Capnography provides breath-to-breath ventilation data Here are five things you should know about waveform capnography.ġ. Capnography offers reliable feedback about the severity of a patient’s condition and how they respond to treatment. Waveform capnography can now be used at all provider levels to better assess patients in respiratory distress, cardiac arrest, and shock. October 3rd, 2018 CapnoAcademy Articles, Capnography 101, Columnists Capnography 101 5 things to know about capnography 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
